Healthcare runs on information. Every diagnosis, prescription, lab result, imaging scan, procedure code, clinic note, and insurance transaction becomes part of a patient’s record. Over decades, this information spreads across many systems — electronic health records (EHR), laboratory information systems, picture archiving and communication systems (PACS), billing platforms, and administrative applications.
When providers modernize infrastructure, merge facilities, replace legacy platforms, or adopt cloud environments, this data needs to follow. That process — moving data safely from one system to another — is known as data migration.
In healthcare settings, migration is rarely a simple technical task. It touches regulatory compliance, clinical workflows, operational continuity, and patient safety. Done well, it enables modernization without interruption. Done poorly, it risks data integrity and everyday operations.
Understanding the healthcare context
At its core, data migration means transferring data from one system, database, or storage environment to another. In many industries, this is primarily a performance or cost optimization task.
Healthcare adds several layers of complexity:
- Regulatory constraints. Patient records are protected under laws such as HIPAA in the United States and GDPR in Europe, which govern how personal and clinical data can be accessed, transmitted, and stored.
- Continuous operations. Hospitals and clinics function 24/7. Systems that support admissions, medication administration, lab reporting, and billing cannot simply shut down for long migration windows.
- Clinical meaning. Data in healthcare is not just numbers — it drives real-time decisions. Error in a dosage, allergy list, or blood type field, even if technical in origin, can affect a clinician’s decisions.
- Heterogeneous environments. Over time, healthcare organizations accumulate multiple systems from different vendors with different data models. Migration often involves consolidating complex, heterogeneous data landscapes.
Together, these considerations shape how healthcare migration is planned and executed.
Typical healthcare data categories
Healthcare systems manage a wide range of data types, some of which include:
- Patient demographics and identifiers
- Diagnoses, procedure codes (such as ICD-10, SNOMED CT)
- Medication lists and allergy information
- Laboratory results coded with standards such as LOINC
- Clinical documentation and encounter histories
- Billing transactions and insurance data
- Audit logs and compliance records
- Binary large objects (BLOBs) linked to document repositories or imaging metadata
Large healthcare providers may operate databases measuring in terabytes. Migration solutions must handle both high-volume structured data and large BLOBs without degrading performance or accuracy.
Regulatory and security foundations
Patient information is highly protected. Regulations require that data be secured during transit and at rest, access be narrowly controlled, and actions be auditable. Healthcare migration is not an exception — it is already part of the compliance mandate.
From a security perspective, migration introduces several risk points:
- Elevated access rights required to read and transfer sensitive data
- Increased exposure when using intermediary systems or middleware
- Possible interception of data in transit
- Operational risks if production systems are overloaded during migration
To address these concerns, migration architectures should aim for simplicity and security:
- Secure direct connections between source and target environments
- Read-only access to production systems
- Encryption in motion
- Strict role-based permissions
- Monitoring and logging for audit purposes
Clear governance, well-defined procedures, and secure tooling reduce exposure and support compliance throughout the migration lifecycle.
Preserving continuity of care
Patient care cannot pause while data is being transferred. Clinicians need uninterrupted access to information such as:
- Active medication records
- Recent laboratory values
- Current allergies
- Recent imaging studies
Traditional offline migration models, where systems are taken offline for an extended period, are rarely acceptable in hospitals or large clinics. Instead, phased approaches are used:
- The bulk of the historical data is transferred first
- Ongoing changes are continuously synchronized
- A short, controlled final cutover window is planned
This approach limits disruption and ensures that clinical systems continue to deliver timely information throughout migration.
Data mapping and structural alignment
Reliable migration requires careful preparation prior to data transfer. Data fields between source and target systems often differ in structure, naming, type, or length. Subtle misalignments — different date formats, numeric precision, or character encoding — may introduce errors if not reconciled.
Data mapping is the process of defining how each source field corresponds to its partner in the target schema. This work ensures that:
- Clinical meaning is preserved
- Units of measure remain consistent
- Values do not get truncated or corrupted
- Field formats align with target system expectations
While migration technology handles the process of moving data, the quality of the preparation — the schema alignment and mapping — underpins the effectiveness of the migration.
Handling legacy data
When healthcare organizations choose to migrate data, they often face a decision: move everything into the new system, or archive some legacy records?
A full historical migration delivers a unified data set but increases the scope and complexity of the project. On the other hand, maintaining historical data in a read-only archive reduces the load on the new operational database but requires reliable archival access mechanisms for compliance or research.
A balanced strategy is common:
- Recent and active records are migrated into the new system
- Older data is archived and accessible through secure archival services
The choice depends on regulatory retention requirements, clinical needs, reporting obligations, and budget constraints. Deciding early helps define technology, performance expectations, and validation scope.
Healthcare data migration tools
Because of the complexity, scale, and regulatory sensitivity of healthcare environments, purpose-built migration tools are preferred over ad-hoc scripts or manual exports.
Effective healthcare migration tools typically offer:
- Secure, direct database-to-database transfer
- Support for high data volumes and large binary objects
- Continuous synchronization between source and target systems
- Parallel data loading for faster throughput
- Robust monitoring and recovery options
- Minimal architectural complexity
One enterprise-grade solution in this space is Ispirer Data Migrator.
Ispirer Data Migrator in healthcare contexts
Ispirer Data Migrator is designed specifically to support data migration (not schema conversion) in demanding environments. It transfers data into a prepared target schema through secure connections, without altering production systems.
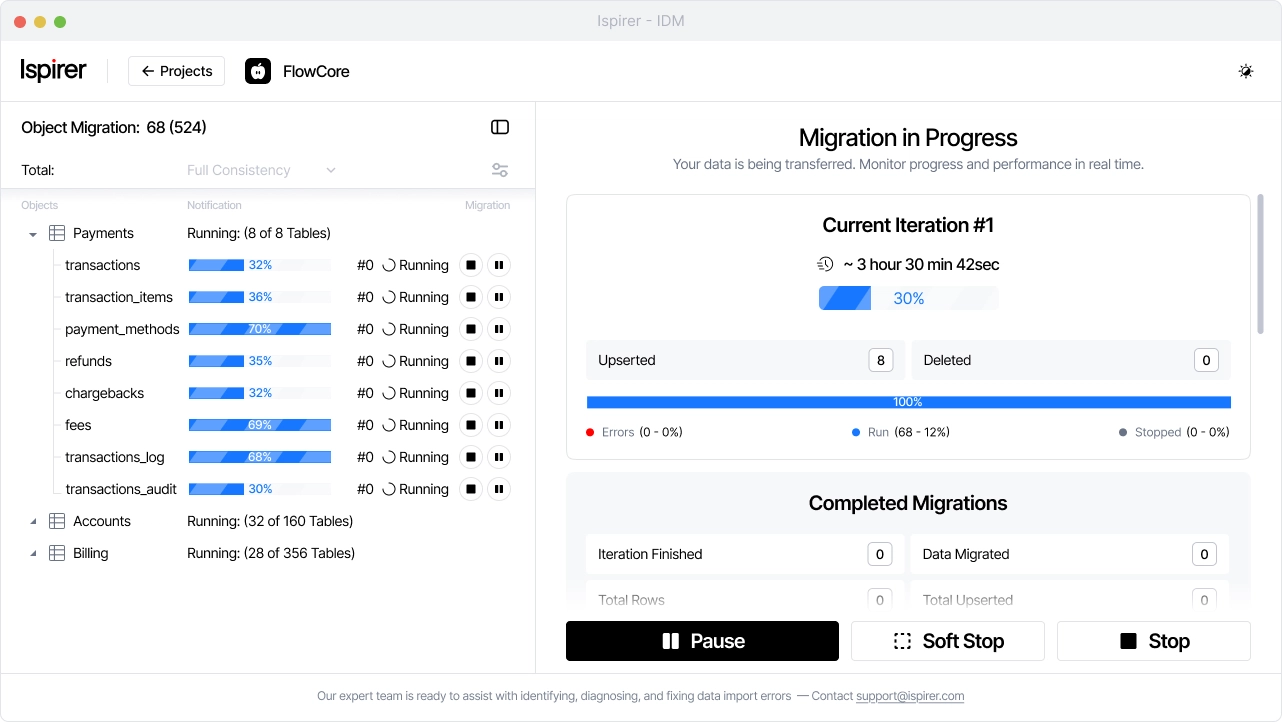
Key characteristics relevant to healthcare include:
- Read-only access to source systems: This protects operational stability, ensuring production databases remain unchanged during migration.
- No middleware requirement: Direct transfer reduces architectural complexity and limits potential exposure.
- Near-zero downtime through continuous synchronization: Built-in replication keeps the target system in sync with ongoing changes in the source, shortening final cutover windows.
- Parallel processing: Multiple data streams run simultaneously, improving performance over single-threaded approaches.
- Support for diverse data types, including large BLOBs: Healthcare data often includes large object references, and efficient handling of these is essential.
Because Ispirer Data Migrator focuses strictly on transferring data, it can be paired with schema conversion tools, like Ispirer SQLWays, and validation processes that prepare the target environment in advance.
Best practices for healthcare data migration
Technology choices matter, but execution discipline and governance ultimately determine success. The following practices support accurate, secure, and disruption-free data migration in healthcare environments:
Start with a detailed data inventory
Before moving any data, identify exactly what will be migrated. Map all source systems (EHRs, billing platforms, lab systems, imaging repositories), estimate data volumes, define active vs. archived datasets, and understand data relationships. Clarify which records must be migrated in full, which can be summarized, and which may remain in legacy systems for compliance access only. A precise inventory reduces scope creep and unexpected delays.
Define clear data mapping rules
Data migration requires explicit mapping between source and target fields. Even if systems are structurally similar, naming conventions, formats, and value sets may differ. Define transformation logic for date formats, identifiers, codes, units of measurement, and status values. Document how null values, duplicates, and historical versions of records will be handled. Clear mapping rules prevent inconsistencies and data misinterpretation.
Clean and prepare data before migration
Migrating inaccurate or duplicate records transfers problems into the new system. Perform data profiling to detect anomalies, missing values, and inconsistencies. Remove obsolete entries where appropriate, standardize terminology, and resolve duplicates. Clean data improves reporting accuracy and system performance after migration.
Use staged testing in non-production environments
Conduct multiple trial migrations in development or staging environments. Test with representative datasets to validate performance, completeness, and data integrity. Compare source and target record counts, key identifiers, and sample patient histories. Testing in controlled environments helps identify issues without affecting patient care.
Monitor migration progress in real time
During execution, track transfer progress, throughput, error logs, and failed records. Implement automated alerts for data mismatches or replication interruptions. Continuous monitoring allows teams to intervene quickly if unexpected issues arise.
Plan cutover carefully
Define the exact point at which users switch from the source system to the target system. Establish data freeze periods if necessary to prevent inconsistencies. Communicate clearly with clinical and administrative teams about expected timelines and access limitations. A well-coordinated cutover minimizes disruption to care delivery.
Prepare rollback procedures
Even with careful testing, issues may arise. A rollback plan defines how to revert to the original system safely if validation fails. This includes preserving backups, maintaining data integrity checkpoints, and defining decision authority during go-live.
Perform comprehensive post-migration validation
After migration, verify that all expected records were transferred accurately. Reconcile record counts, confirm patient identifiers, and test critical workflows such as medication review, lab result lookup, and clinical documentation retrieval. Validation should include both technical checks and user acceptance testing.
Ensure regulatory compliance throughout the process
Healthcare data contains protected health information (PHI), so migration must comply with HIPAA, GDPR, or other applicable regulations. Encrypt channel for transition, restrict access to authorized personnel, maintain audit logs, and document every migration activity for compliance review.
Engage clinical stakeholders early and often
Clinicians and operational staff should participate in validation to confirm that migrated data appears complete, accessible, and usable within real workflows. Their involvement ensures that migration success is measured not only technically, but also operationally.
Document every step of the migration process
Maintain detailed records of mapping rules, validation results, reconciliation reports, and approvals. Documentation supports audits, regulatory reviews, and future system transitions.
Migration as part of broader transformation
Data migration does not, by itself, transform clinical practice or improve health outcomes. What it does is enable modernization.
By moving data into stable, scalable, and performant environments, healthcare organizations position themselves to adopt:
- Scalable cloud infrastructure
- Advanced analytics and reporting
- Interoperability with external providers and public health systems
- Efficient disaster recovery capabilities
Reliable migration ensures that modernization initiatives build on a solid foundation rather than disrupt daily operations.
Final thoughts
Healthcare data migration sits at the intersection of technology, clinical practice, and regulatory compliance. It challenges organizations to preserve clinical accuracy, safeguard patient privacy, maintain continuity of care, and modernize infrastructure simultaneously.
Successful migration combines disciplined planning, secure and capable technology, and careful validation. Solutions such as Ispirer Data Migrator provide enterprise-grade capabilities for secure, high-volume data transfer with near-zero downtime, while allowing organizations to focus on clinical readiness and operational continuity.
When the right strategy, stakeholders, and tools come together, healthcare data migration becomes less of a risk and more of a well-managed step toward sustainable digital transformation.












